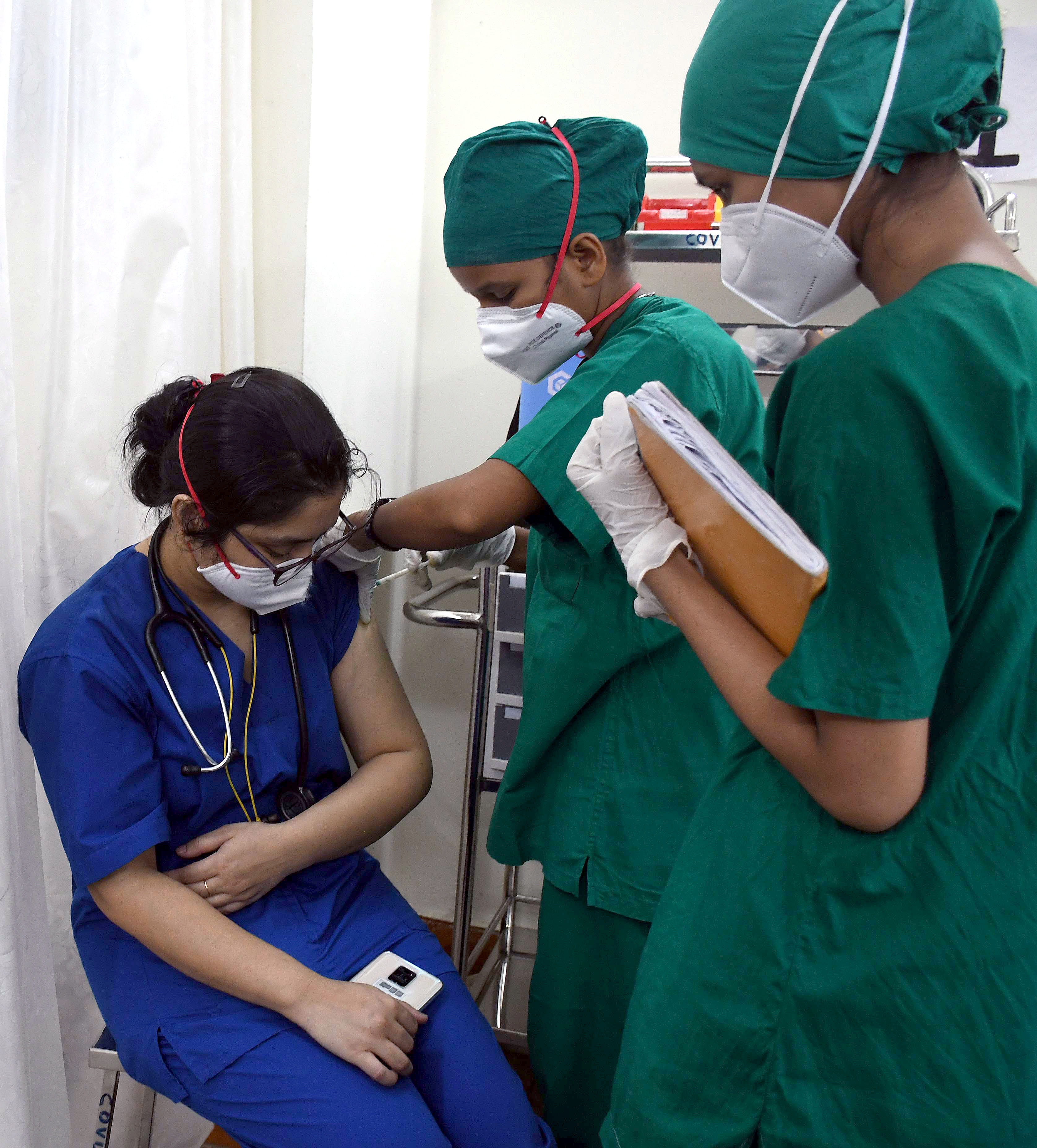
The speed of this surge was so rapid and the scale so astronomical that any health system in the world would be challenged.
As the SARS-CoV-2 virus (Covid-19) relentlessly continues its march of death and devastation across the country and as oxygen supplies dwindle, available hospital beds become scarce and bodies pile up in front of crematoriums, India finds itself engulfed in a welter of emotions ranging from anger, despondency and sheer helplessness.
Pertinent questions swirl around. Where did we go wrong? Was it inexcusable incompetence laced with an unhealthy dollop of overconfidence that was our undoing? Had we become too complacent? Or were there factors that were beyond the realm of human predictability?
What do we do now?
There are no black and white answers to these relevant queries. The truth lies somewhere in between.
The first wave of the virus dealt India a relatively favourable hand. Despite India registering its first case as early as January 2020 in concert with the rest of the world, India experienced a relatively low caseload and a low fatality rate. India’s age demographics (larger number of young people), the stringent lockdown enforced by the Narendra Modi government in the early phase of the pandemic and the innate immunity of Indians were possible factors that effected a better outcome.
By February 2021, the situation appeared to be in control. From a peak of nearly 100,000 cases per day in mid-September (17 September, 97,894), the country had seen a steady decline with numbers falling to around 11,000 in early February.
Research studies conducted in December and January pointed to a significant level of herd immunity. In some areas of India’s major cities, the antibody positive rate (an indicator of immunity) was in excess of 50%. On a national level the studies revealed that nearly 271 million or one-fifth of India’s population had been infected.
Experts indicate that a herd immunity rate of anywhere between 50-90% may be required to see a decline in infection rates depending upon the contagiousness of the diseases.
Understandably, a sense of complacency set in. Complacency led to a lowering of our guard; adherence to social distancing and mask wearing decreased. Humungous gatherings like the Kumbha mela were allowed to occur and election campaigns proceeded unchecked.
Then all of a sudden, the tide turned. Beginning in late February coronavirus cases began to mount—slowly at first and then skyrocketed. In a period of just over a month, Covid-19 cases escalated sharply from 24,882 per day (13 March) to an astounding 345,882 cases (25 April)—nearly 3 times the previous peak reached in September and besting every peak level seen in any other part of the world. The highest number of daily
The speed of this surge was so rapid and the scale so astronomical that any health system in the world would be challenged. India’ s healthcare infrastructure, shaky and deficient even at best of times has been expectedly pushed to the brink: oxygen is in short supply, hospital beds are scarce and essential medications are running low. India’s predicament is no different to what even New York, a city with a robust health network underwent in March last year. Stretchers lining the corridors of hospitals, ventilator shortages, dearth of medical supplies and refrigerated trucks serving as impromptu morgues became commonplace. Therefore, to expect complete preparedness for such a catastrophic calamity is a bit too optimistic.
Nevertheless, apart from public complacency there have been administrative lapses that have added to our misery. While the political leadership must ultimately accept responsibility for happenings under its watch, there are other layers of responsibility that need to be analyzed for failure.
In March 2020, the Modi government had constituted 11 empowered groups headed by experts to plan and manage the spread of the novel coronavirus. Later in September these 11 groups were consolidated into six larger groups to deal with various issues, including medical infrastructure and pharmaceutical supplies.
The question then arises whether these expert groups failed to identify and warn the government in a timely manner of this impending crises.
Next, there also appears to be a failure at the state level as well. Justices Vipin Sanghi and Rekha Palli of the Delhi High Court came down heavily on the local government for its handling of oxygen shortage during the Covid-19 crises: “Set your house in order. Enough is enough. If you cannot manage it, tell us, then we will ask the Central government to send their officers in and do it. We will ask them to take over. We cannot let people die like this.”
However, to indulge in a blame game at this juncture would be suicidal. The need of the hour is a determined effort to combat the crises. The government on its part has swung into crisis mode after a period of hesitancy. To offset the oxygen shortage, non-medical use of oxygen has been banned, IAF and Indian Railways have been pressed into service to transport oxygen cylinders and more oxygen is being procured from abroad. Field hospital like the 500-bed Covid-19 center in Delhi manned by the ITBP have been set up in several places. Aid in the form of medical supplies from abroad has been pouring in. Let us hope that this will be bring more stability to medical establishments so that they are better equipped to treat Covid-19 patients in the days to come.
But the bigger problem that lies ahead is the prevention of the spread of the virus. Central to this goal are increased testing, universal mask coverage and aggressive vaccination.
Modelling statistics paint a grim picture for the immediate future. The Institute for Health Metrics and Evaluation (IHME), an independent global health research center at the University of Washington predicts that the death toll in India will likely double to 665,000 by 1 August 2021, reaching a peak of 5,600 deaths per day on 10 May. Universal mask coverage implemented almost immediately will serve to decrease the death toll by 70,000 and aggressive vaccination will reduce the deaths by another 85,000.
As of 27 April, only 147.7 million doses of Covid-19 vaccines have been administered. In terms of percentage this number is rather disappointing: only about 2% of Indians have received both doses and about 10% have received at least 1 dose. At the current rate of vaccination, only 30% of the eligible population will be vaccinated fully by the end of this year. If India wants to reach a herd immunity of 80%, it needs to increase its vaccination rate by about 100 million doses/month. To meet this increased demand the government has funded the Serum Institute of India (SII) and Bharat Biotech to increase their production and has made arrangements to import vaccines from other countries as well. But to make the current vaccination plan more effective the government must give consideration to universal vaccination free of cost.
With an accelerated vaccination drive on the part of the government and public buy in for social distancing norms such as universal mask coverage, India will hopefully manage to bring this scourge under control by the end of the year.